Nursing scheduling is notoriously a difficult task for any HR department. There are many factors to keep in mind to deliver the best patient care possible while supporting staff: managing shift swaps, call-outs and vacations.
Fostering a positive, seamless environment allows staff to perform their best and enhance job satisfaction, directly improving patient care.
To give you the best chance of success, we’ve outlined important trends to watch out for when planning your nursing schedule in 2024 and beyond. We’ll cover the importance of a successful nursing schedule and provide solutions to any probable challenges to expect when managing a nursing schedule.

What is important when creating a nurse schedule?
First, let’s talk about what a nursing schedule is. It’s a plan that outlines the working hours, shifts and assignments for nurses over a specific period (usually on a weekly or monthly basis). A schedule helps you to provide suitable staffing levels to deliver appropriate patient care.
You can use scheduling to assign patients to the most-suited nurses. For example, if a nurse has years of experience working with dementia patients, it’s beneficial to allocate them to a patient diagnosed with dementia.
Here are some of the typical elements to include in a nurse’s schedule:
- Shifts: The set amount of time your nursing staff are working.
- Shift duration: The start and end time of each shift.
- Assignments: Any tasks or activities assigned to nursing staff during their shifts.
- Staffing levels: Whether you’re overstaffed or understaffed.
- Rotation patterns: If staff work schedules that are allocated to them on a routine basis.
- Breaks: When each staff member has their scheduled rest period during their shift.
- Days off: Days when staff members are required to have a break between shifts (based on employee regulations in your area).
- Shift changeovers: Periods where nursing staff hand over to other staff members before they finish their shift.
- Overtime: When members of staff work beyond their contracted hours.
- On-call times: When members of staff aren’t working but are expected to be contactable in emergency circumstances.

How does effective scheduling benefit nurses?
Let’s take a look at some of the benefits of creating a successful nursing schedule in a healthcare organization.
To provide the best level of care
Scheduling issues are a common problem for nursing staff. When there isn’t enough staff working, it affects patients’ level of care and puts stress on those who are working. Each patient requires and deserves a high level of care, including dressing, washing, medicating and transporting from their room to the food hall and back again. So there should be an appropriate patient-to-staff ratio to deliver the best care.
On average, each nurse requires eight hours to deliver the best care possible in a busy nursing home. This doesn’t include breaks, and it means that patients only ever get to see their room and the food hall. The nurses are unable to tend to their other personal needs or take them outside, which results in suboptimal patient care.
In this situation, a nursing schedule would help to manage tasks efficiently and show if/where you need support and on what particular days.
To prevent burnout
Without a schedule in place to share the load of work, you risk overworking nurses.
Let’s say there are only four nurses scheduled during a peak shift when there should be six. Those four nurses are carrying the weight of an extra two people, meaning they’re overworking, likely at their peak mental capacity and aren’t able to perform each task with 100 percent attention and a high level of care.
Being overworked also means that nursing staff are unlikely to deliver the level of care they’d like. This can impact morale and also lead to injury — for the nurse and the patient.
For example, let’s say a member of your nursing staff covers another shift due to scheduling issues. They’re asked to safely lift and move a patient. Because they’re so tired from overworking, they don’t have the energy to perform the maneuver correctly. This can increase the risk of injuries to both parties, which could then lead to further staffing issues.
To improve efficiency
Scheduling tools keep healthcare organizations running efficiently, giving everyone a clear picture of their day and allowing nurses to focus on their work.
A well-structured schedule also covers break times and shift changeovers. This minimizes disruptions, allowing nurses to provide continuous and uninterrupted care to patients.
Plus, you can also improve continuous care, which means patients receive supervision from the same nurse or team of nurses. All staff members will know what they’re expectations are and when to perform them.
To follow laws and healthcare regulations
Compliance with labor laws and regulations surrounding nurse scheduling is crucial. Doing so ensures proper rest periods, meal breaks, safe working conditions and adherence to overtime rules. Here are some examples*:
- If an employee works over five hours in Colorado, they’re entitled to a 30-minute break.
- Mandatory overtime is prohibited or limited in 18 US states, with maximum shift allowances based on your location.
- Some state laws (including Massachusetts) require one nurse per patient in the intensive care unit. There are some exceptions if a patient is stable enough to pair with more than one nurse.
With effective nursing scheduling, you won’t overwork nurses and operate within the law. You can allot time for breaks and ensure there are enough staff working every day to prevent unnecessary overtime.
*These are just a few examples. Be sure to check your local state and government websites to understand the regulations for your healthcare organization.

What are the challenges of nursing scheduling?
Let’s walk through some of the common hurdles that healthcare administration professionals face when scheduling shifts for nursing staff.
- Managing staffing levels: Overstaffing can lead to unnecessary labor costs, while understaffing can increase stress, jeopardize patient safety and impact the quality of care.
- Shift preferences: Juggling preferences for specific shifts or vacation days while making sure you have adequate staffing levels can be difficult for HR professionals to balance.
- Nursing skills: Allocate nurses according to patient needs and, in some cases, sometimes preferences. This means you often need a mix of nursing skills to deliver the appropriate level of patient care, which can be tricky to manage.
- Scheduling conflicts: Conflicts can appear when multiple nurses request the same vacation days or if there are overlapping preferences for shifts. Managing these requests to prevent any conflicts and ensure all staff members are happy can be tough.
- Emergency situations: Unexpected events (such as pandemics or natural disasters) can disrupt regular scheduling. In this situation, your schedule requires rapid adjustments, which can be stressful to organize.
What is a typical nurse schedule?
A typical nursing schedule varies based on different factors, such as the type of nursing, nurse availability, state requirements for patient care (such as one nurse to two patients in the ICU, like in California) and so on.
However, there are some common shift patterns for nurses across the United States. Let’s take a look at how they work.
Eight-hour shifts
An eight-hour shift is probably the most common shift for nurses, and nurses typically complete five consecutive eight-hour shifts before having a couple of days off. Then, they’ll come back to work for the next rotation of eight-hour shifts.
Eight-hour shifts can be broken into three main patterns:
- The day shift typically runs from early morning (7 a.m.) to late afternoon (3 p.m.).
- The evening shift generally starts in the late afternoon (3 p.m.) and ends in the evening (11 p.m.).
- The night shift usually begins in the evening (11 p.m.) and ends in the early morning (7 a.m.).
12-hour shifts
Nurses also work 12-hour shifts, depending on your state’s maximum shift duration allowance, rotating between days and nights that are typically on a two–three-day rotation. Then, they have the rest of the week (usually four days) to recharge and enjoy some downtime.
State requirements vary for the required amount of time to rest between 12-hour shifts. For example, the California Labor Code requires that employers pay nurses time-and-a-half for any work over eight hours in a 24-hour period.
In Pennsylvania, an employee who works more than 12 consecutive hours can get 10 consecutive hours of off-duty time immediately following their shift. However, employees can reduce this off-duty time if they wish.
Oregon also has a secure scheduling law, which requires employers to provide a 10-hour rest period between shifts.

Nursing scheduling: Trends to watch in 2024 and beyond
There are a lot of trends impacting the nursing and healthcare industry in 2024. Here are the three that we think are at the top of the list:
- Artificial intelligence (AI) and digitalization: Technology is constantly evolving in the healthcare industry. Using AI to predict staffing needs is just one example of how digitalization is influencing the way HR professionals create and manage nursing schedules.
- Predictive analytics: The growing use of predictive analytics allows HR professionals to analyze historical data to make informed decisions about scheduling and shift patterns. In doing so, you can improve your scheduling, better allocate resources and, ideally, offer patients a better level of care.
- Staffing shortages: The lack of nursing professionals isn’t a new trend, but it’s still impacting the industry. For HR professionals, it can limit the number of nurses available and how high your turnover is. With the right tactics in place, you can boost retention and make it easier to plan your nursing schedules.
Let’s look at these trends in more detail, including how to incorporate them into your own scheduling process.
AI and digitalization
For a while, digitization was a popular trend in healthcare — it’s the process of converting physical information into digital formats. There’s been a shift from pen-and-paper data management toward automation, which involves using technology to improve your operations and offer more value to your patients.
In fact, the World Health Organization outlined this in the Global Strategy on Digital Health 2020–2025, showing just how significant it is.
Research has found that the digital health market could reach nearly $660 billion by 2025, up from $179 billion in 2019. Artificial intelligence is also a growing trend to look out for. The AI healthcare market was worth around $11 billion in 2021 and is expected to hit almost $188 billion by 2030.
Take a look at Sanford Health, as an example. The organization has been adopting AI tools to predict staffing needs and schedule nursing shifts.
But it’s not just AI that’s helping healthcare facilities improve their processes. With digital tools, HR professionals can easily make changes to nursing schedules, get a clear overview of shifts in real time and even collaborate with nurses virtually to create a schedule that works for them.
Review your current processes to identify areas that digitalization can improve. The whole idea behind digitalization and AI is to take some workload off of your hands and make your life easier, so make the most of it.
For example, let’s say that you’re struggling to manage overtime thresholds. By identifying this issue, you could find a platform that sets overtime alerts (something which we offer at Empeon). That way, you can use technology to keep on top of overtime hours and make sure your schedules are up to date.
Upgrading your digital infrastructure doesn’t have to be complex. There are plenty of tools out there that make it easy for healthcare professionals to digitize their scheduling and other healthcare processes.
For example, HR and payroll solutions like Empeon. With our software, you can onboard new staff, manage payroll and streamline nurse scheduling within a single platform.
Predictive analytics
Predictive analytics — or predictive analysis — involves using past data to predict future trends. This includes monitoring patient symptoms, tracking the number of patients coming into the facility at certain times and recording their stay duration.
Figures show that the predictive analytics market is expected to grow from now until 2030 at a compounded annual growth rate (CAGR) of 24.4 percent. Plus, in 2022, 66 percent of US healthcare leaders used predictive analysis.
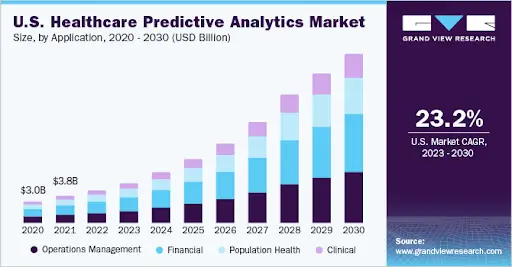
In healthcare, the demand for predictive analysis has been the result of a drive to improve patient outcomes, provide high-quality healthcare and reduce costs.
For example, you can forecast patient demand based on previous historical data and trends. As a result, you can schedule nurses more efficiently, reduce understaffing or overstaffing issues and provide patients with the utmost care when they need it.
Take a look at some of the ways you can incorporate predictive analysis into your healthcare facility:
- Find the right platform: Start by finding a predictive analytics platform that works for your organization. Figure out what features you require and your budget. If you’re not sure what you’re looking for, some helpful features to consider include data analysis (so you can analyze key trends and allocate staff and resources effectively), automation (so you can instantly schedule staff) and electronic health records (so you can track key patient data to inform future schedules).
- Choose the algorithms: Decide which data you want the software to analyze to help you update your nursing schedule. For example, you might want to identify peak periods when you need more nurses on shift. Depending on the platform you use, you can often create dashboards that display this information clearly. Then, you can use these insights to schedule shifts accordingly.
- Consider scalability: When you first start using predictive analytics, you might begin by analyzing the volume of patients coming into your facility. Over time, you realize that you also want to analyze patient symptoms and duration of stay. Plus, you may want to integrate existing software (such as payroll and HR platforms) to streamline your operations. This means choosing scalable software that’ll support your organization as your needs evolve. Spend some time reviewing all the features of the software, even if they’re not relevant to your organization right now. In time, these features might be what you need to improve your scheduling and deliver top-quality patient care.
Staffing shortages
Staffing shortages are a long-term trend that’s affecting the healthcare industry. In 2017, the Health Resources and Services Administration predicted the requirement for a million new nurses in the next 10 years. The same study forecasts there’ll be a 13 percent shortage of nursing staff by 2030 to meet that demand.
And although the great resignation is over, the effects of the pandemic still impact nursing today. A study from 2021 found that 40 percent were satisfied with being a registered nurse, compared to 62 percent in 2018. By 2027, almost 900,000 nurses plan to leave the profession.
These figures mean that you need to consider nursing staff’s happiness and well-being when scheduling shifts. As a result, you’re more likely to offer nurses a better work experience, increasing their happiness at work and boosting retention.
Here are some ways to keep nurses happy so they stick around:
- Offer flexibility: Create a healthy work-life balance for staff by offering some level of flexibility with shifts. For example, if an employee asks not to be scheduled on a Friday so they can take care of their children, do your best to make this happen. You might not be able to promise this every week, but do your best to provide some flexibility.
- Provide support: As an HR professional, you can provide support for nurses by offering regular check-ins and open channels of communication to address any concerns. This shows them that they have access to support as and when they need it. You can also offer professional development opportunities and resources to help nurses enhance their skills, develop their career and feel more confident in their abilities.
- Manage payroll and HR effectively: Give your staff one less thing to worry about by using an efficient and accurate payroll software and HR system. Having this in place can motivate staff and let them know you’ll always pay them accurately and on time. Plus, it makes it easy to track working hours and overtime, providing them with transparency of what they’re being paid for. This also builds trust with your staff, which has been shown to boost retention.
Utilize technology to improve the HR experience
From predictive analysis and artificial intelligence to staffing shortages and retention rates, there’s a lot to consider when it comes to managing shift schedules for your nursing staff.
One of the biggest and constantly evolving trends is the use of technology. The right digital infrastructure can elevate the nursing experience and help you provide a better service to patients.
To start building a successful digital set-up, take a look at Empeon. Our software makes it easier for you to ensure HR compliance, safely store employee data and streamline your time management and scheduling.
Get in touch with one of our industry experts to learn more.



